Oral Surgery in Jacksonville Beach – Jax Beaches Family Dentistry
We provide state-of-the-art oral surgery services conveniently located in the Jacksonville Beach – Neptune Beach – Atlantic Beach area and serving all of Greater Jacksonville.
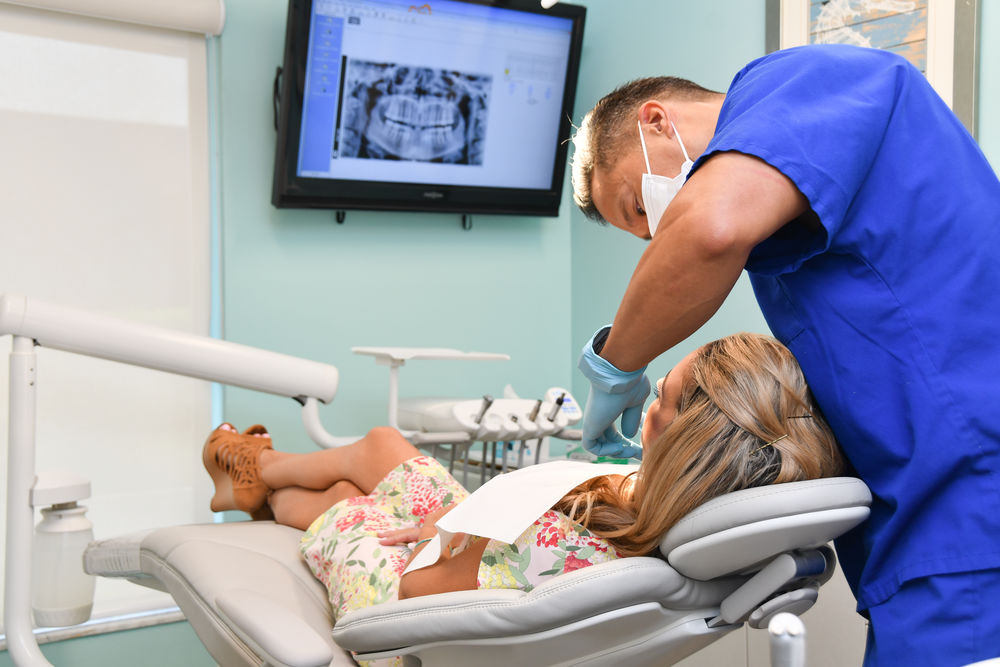
Repair Your Smile
Jax Beaches Family Dentistry provides innovative care based upon years of training and experience. We offer a full scope of oral and maxillofacial surgeries. Regardless of complexity our goal is the same – compassionate care that delivers renewed and beautifully fully-functioning smiles.
Oral & Maxillofacial Surgery
Jax Beaches Family Dentistry’s Dr. Stephen Strout is one of Florida’s leading periodontists having successfully performed thousands of often complex oral surgeries. We are proud to have him on our Team.
Wisdom Teeth Removal
Most people’s mouths only have enough room for 28 teeth. If you have wisdom teeth, that’s four additional teeth trying to cram their way into a space not meant for them. This often creates problems, including crowding, soreness, risk of infection, and the need for extraction. We can determine if your wisdom teeth are impacted and need to be removed. Because wisdom teeth rarely come in straight and consistent with the rest of your smile, we often have to extract them. Of note, wisdom teeth also can come in “sideways,” causing even more problems. Call Jax Beaches Family Dentistry today to schedule your appointment for a wisdom teeth analysis or extraction.
Dental Implants
Dental implants are changing the way people live. They are designed to provide a foundation for replacement teeth that look, feel, and function like your natural teeth. With a dental implant you will be able to eat anything. Replacing missing teeth with dental implants preserves and restore more “youthful” facial contours. Patients with dental implants can smile and eat with total confidence.
The dental implants themselves are tiny titanium posts surgically “implanted” into the bone where your teeth are missing. These metal anchors act as tooth root substitutes. The bone bonds with the titanium “posts,” creating a strong foundation for artificial teeth. Abutments – or small posts allow artificial teeth to be attached to the implant. Implants also help preserve facial structure, preventing bone deterioration that occurs when teeth are missing.
For most patients, the placement of dental implants involves only one surgical procedure.
If you are having an extraction, the tooth is removed, and the implant is placed into the socket during the same procedure. A healing abutment is placed to contour the gum tissue for the tooth restoration. The implant can heal in approximately 6 weeks, at which time you will return to the office for a quick evaluation and clearance to proceed with the restorative phase. Typically, we do not even need to “numb up” after your initial surgery!
When front teeth are involved, temporaries must be fabricated to assist with the obvious social issues.
At times, patients may have poor quality bone or insufficient volume of bone. In these cases, the surgeon may elect to allow the implant to heal beneath the surface of the gum for additional protection. After the implant has bonded to the bone, the second phase begins. Our physicians will uncover the implant and attach a small healing cap that protrudes through the gums. This will help shape the gingiva, resulting in a more cosmetic result. The restorative phase then begins.
When the artificial teeth are placed, the implant components will not be seen. Most patients experience minimal disruption in their daily lives. In most cases, patients can easily return to work the following day after surgery. Postoperative discomfort is considered minimal.
Bone Grafting
Jawbone deficiency can arise from various oral health problems or as a result of multiple dental issues occurring simultaneously. The most common problems resulting from a decrease in the height and width of the jawbone include when you are missing a tooth and do not replace it in a timely manner. When that occurs, the jawbone does not receive proper stimulation from activities such as chewing. Consequently, it begins to decrease in size and strength in the area that previously anchored the tooth root. The rate of deterioration varies greatly among individuals, making it difficult to determine the amount of jawbone loss an individual has suffered without proper examination. In general, jawbone resorption usually begins to occur immediately following the loss or removal of a tooth and continues to worsen as time goes on.
Periodontal disease is one of the most common reasons for eventual bone grafting. There are two major types of periodontal disease: gingivitis and periodontitis. Gingivitis is primarily caused by dental plaque — the bacteria and food particles that accumulate in your mouth on a regular basis. If the teeth aren’t cleaned properly with routine hygiene efforts, the bacteria in the plaque can create swelling, inflammation, the formation of pockets in the gums (which are difficult to clean and begin to house more bacteria), and the formation of tartar (hardened plaque). If gingivitis is not treated properly, it can progress to a more severe infection — periodontitis — which causes the supporting gum tissue and bone holding the teeth in place to deteriorate and leads to tooth loosening and, ultimately, tooth loss.
Unlike dental implants, unanchored dentures and bridgework do not replace the missing tooth root and contribute to jawbone deterioration. Unanchored dentures are placed on top of the gum line and lack the ability to provide direct stimulation to the jawbone. The inevitable bone loss can lead to loosening of the denture, problems speaking and eating, and the need for a stronger adhesive or even a full new set. Bridgework is attached to two healthy teeth stimulating growth; however, the area over which the bridge spans cannot properly stimulate the underlying jawbone. A bone grafting procedure can halt and correct the jawbone damage caused by these prosthetic options.
It is not uncommon for individuals to need a bone grafting procedure as a result of a birth defect. Conditions characterized by missing bone in the teeth, facial bones, jaw, or skull can be treated with this technique to replace the missing bone and stimulate healthy bone growth following the procedure. This can also be used to treat individuals who develop a sinus deficiency in the upper jaw that can occur following molar removal. As the sinuses become enlarged, the height of the jawbone decreases, and a bone grafting procedure may be necessary to replace the missing tooth with a dental implant.
There are various bone grafting techniques that can be used to restore jaw function, and the type of bone used will depend on the specific needs of each patient.
Tooth Extraction
When teeth become damaged by decay or break down due to trauma or wear, they can typically be restored with a filling, root canal, or crown. When the damage is too great, we may decide that the best course of action is to have the tooth removed. If this is the case, we will develop a plan for extraction, taking into consideration your age, health, and the overall condition of your mouth. Most teeth extractions can be performed in one visit to Jax Beaches Family Dentistry.
Some common reasons that a tooth may need to be extracted include:
Crowding. There are times when seemingly healthy teeth need to be removed. Occasionally we are born with too many teeth, or our mouth is too small for all the teeth we have.
Infection and decay. If a tooth is decaying, it is important to have it treated in the early stages when it can be repaired with a dental filling. If left untreated, decay continues to spread and affect the integrity of your tooth, which may now require root canal therapy, a crown, or extraction.
Loose teeth. Many patients are affected by periodontal or gum disease. Left untreated, periodontal disease may cause teeth to shift, become loose, or lead to serious infection and require the removal of a tooth or multiple teeth.
Trauma. Teeth may be fractured or broken due to an accident. If there isn’t enough structure remaining for a filling or crown, your dentist may recommend that the rest of the tooth be removed.
When having a tooth extracted at Jax Beaches Family Dentistry you will undergo a thorough oral exam. Factors including age, the presence of gum disease, and the tooth’s relationship with other areas of the mouth, such as your sinuses, nerves, and other teeth, will be taken into consideration when developing our extraction plan.
Most tooth removals can be completed during a single visit, in which the evaluation and removal are performed at the same time. Most tooth extraction procedures are completed using a local anesthetic to mitigate any pain, and our patients can return to work or their daily activities following their extraction.
Emergency Periodontist / Oral Surgery Services
A loose dental implant?
If your dental implant feels loose, we’ll have you come to our office so we can determine the cause. Usually when a dental implant seems loose, it’s actually the healing abutment or restoration attached to the implant (the crown, bridge, or denture) that is loose, not the implant itself. However, if it is the implant that is loose, prompt care is needed in order to save it.
How do I get an emergency dentist or oral surgery appointment?
If you need an emergency appointment, call our office as soon as possible.
Can you get emergency wisdom tooth removal?
If there is an emergency or infection related to a wisdom tooth, the sooner it’s treated the better. If you believe one or more of your wisdom teeth is infected, call our office NOW to schedule an appointment.
How do you know if you have a wisdom tooth infection?
The most common symptom of a wisdom tooth infection is pain. You may also have an abscess, which is a small, pimple-like bump on the gums near the affected tooth. An infected wisdom tooth produces constant, throbbing pain that radiates to the head and jaw. You may also notice that the tissue surrounding the tooth is warm and swollen and you might have a foul odor or discharge in your mouth.
Will Your Periodontist pull an infected tooth?
Periodontists can pull infected teeth, but your situation will be carefully evaluated before we suggest treatment.
Sleep Apnea Solutions
People with obstructive sleep apnea (OSA) have disrupted sleep and low blood oxygen levels. When obstructive sleep apnea occurs, the tongue is sucked against the back of the throat. This blocks the upper airway and airflow stops. When the oxygen level in the brain becomes low enough, the sleeper partially awakens, the obstruction in the throat clears, and the flow of air starts again, usually with a loud gasp.
Repeated cycles of decreased oxygenation can lead to very serious cardiovascular problems. Additionally, individuals with this condition will likely suffer from excessive daytime sleepiness, depression, and loss of concentration.
Some patients have obstructions that are less severe called Upper Airway Resistance Syndrome (UARS). In either case, the individuals suffer many of the same symptoms. With detailed sleep test analysis, our doctors at Jax Beaches Family Dentistry can ascertain the level of obstruction and help you address this problem.
TMJ Jaw Disorder Treatment
People who grind their teeth can sometimes develop a serious problem with their jaw, which left untreated, can adversely affect the teeth, gums and bone structure. One of the most common jaw disorders is related to a problem with the temporomandibular joint (TMJ), the joint that connects your lower jaw to your skull, and allows your upper and lower jaw to open and close and facilitates chewing and speaking. TMJ stands for temporomandibular joint, which is your jaw joint. Everyone has two of these: a left and right. TMJ syndrome or TMD (temporomandibular disorder) is a medical problem related to the function of the jaw joint.
People with TMD often have a clicking or popping sound when opening and closing their mouths. Such disorders are often accompanied by frequent headaches, neck aches, and in some cases, tooth sensitivity. Other signs and symptoms of TMD include:
Clicking Sounds — Some people with TMD hear a clicking, popping or grating sound when opening or closing the mouth. This is usually caused by a shifting of the disk inside the joint. Someone standing next to you might even be able to hear it. Clicking by itself is actually not a significant symptom because one-third of all people have jaw joints that click. However, if the clicking is accompanied by pain or limited jaw function — the jaw getting “stuck” in an open or closed position, for example — this would indicate TMD.
Muscle Pain — This can be felt in the cheeks (masseter muscles) and temples (temporalis muscles), where the two big pairs of jaw-closing muscles are located. If you feel soreness and stiffness upon waking up in the morning, it’s often related to habits such as clenching and/or grinding the teeth at night. If you have this type of nocturnal habit, a custom-made night guard could be helpful in decreasing the force applied to your teeth, which will in turn allow your muscles to relax and relieve pressure on your jaw joints.
Once you have been examined at Jax Beaches Family Dentistry, a strategy for treating your TMJ or TMD condition and managing your pain will be developed. Sometimes a temporary change to a softer diet can reduce stress on the muscles and joints. Ice and/or moist heat can help relieve soreness and inflammation. Muscles in spasm can also be helped with gentle stretching exercises. Non-steroidal anti-inflammatory medications and muscle relaxants can also provide relief. Some treatments for TMD include muscle relaxants, aspirin, biofeedback, or wearing a small plastic appliance in the mouth during sleep.
Severe TMD cases may require more complex forms of treatment, which might include orthodontics, dental restorations like bridgework, or minor procedures inside the joint such as cortisone injections or lavage (flushing) of the joint. It’s very rare for major surgery ever to be necessary in a case of TMD.
The Benefits of Seeing a Periodontist for your Oral Surgery Needs at Jax Beaches Family Dentistry
Periodontists perform oral surgeries and are dental doctors who have received years of additional training beyond dental school. Periodontists are qualified to work on the hard and soft tissues of the face and mouth. This can include the teeth, gums, lips, tongue, and upper or lower jawbones.
Why Choose Jacksonville beach Dentistry for your next Oral Surgery?
You have a choice of many dental surgery options in Northeast Florida, but Jax Beaches Family Dentistry offers an effective comprehensive approach to all your dental health needs including the occasional need for oral surgery. Our periodontist, Dr. Stephen Strout has the years of experience and extensive educational background to make certain that your oral surgery experience with Jax Beaches Family Dentistry will be a good one.
Oral Surgery - Frequently Asked Questions (FAQs)
Although the best time for removal of wisdom teeth is about 16 years old, there is a wide age range for patients who require wisdom teeth removal.
Determining when to remove the wisdom teeth involves consideration of:
Age of the Patient: The younger the better. Younger patients typically have less chances of wisdom teeth complications. It is recommended to have your wisdom teeth removed sooner than later if your dentist or our doctors have indicated that conditions are not optimal for keeping your wisdom teeth.
Root Formation:
If your wisdom teeth’s roots have about 1/3rd of formation, this is a good time to consider getting your teeth removed. If you have over 2/3rds root formation on your wisdom teeth, there is an increased chance of complications with wisdom teeth removal.Position of the Tooth:
Another important factor in determining when to remove your wisdom teeth is where the wisdom teeth are positioned relative to other anatomical structures such as the sinuses and adjacent teeth. If the wisdom tooth cannot attain a healthy position then problems can occur such as cavities, infections, or complications with roots.Dental implants are substitute tooth roots used to replace natural tooth roots in areas of the mouth where teeth are missing. Crowns, bridges, or other replacement teeth are then connected to the implants to replace missing teeth.
The reason it is so important to replace the tooth root as well as the visible part of the tooth is so that natural tooth roots are embedded in the bone, stimulating bone growth and providing the stable foundation necessary to bite and chew.
When teeth are missing, the bone that previously supported those teeth deteriorates in a process called bone resorption. However, the bone can be preserved by replacing missing tooth roots with dental implants. Since the bone forms a strong bond to the implants, they can serve the same functions as natural tooth roots.
Overall quality of life is enhanced with replacement teeth that look, feel and function like natural teeth. With implant-supported replacement teeth, the appearance of the smile is more natural and the teeth function more like natural teeth. The result is increased comfort and confidence when smiling, speaking and eating.
Integrity of facial structures is preserved. By preventing the bone resorption that would normally occur with the loss of teeth, the facial structures remain intact. This is particularly important when all of the teeth are missing, as the lower one-third of the face collapses if implants are not placed to preserve bone.
Adjacent teeth are not compromised to replace missing teeth. Tooth replacement with traditional tooth-supported bridges requires grinding down the teeth adjacent to the missing tooth/teeth, so that the bridge can be cemented onto them. This tooth structure can never be replaced, and the long-term health of these teeth is compromised. The teeth are then made to do the work they were intended for plus the work of the missing tooth. Partial dentures have clasps that hook onto adjacent teeth, putting pressure and unnatural torqueing forces on them as the partial rocks back and forth. Eventually these teeth can loosen and come out as a result of this pressure. Replacing missing teeth with implant-supported crowns/bridges does not involve the adjacent natural teeth, so they are not compromised or damaged.
- The mouth is restored as closely as possible to its natural state. By replacing the entire tooth, including the root, it is possible to replicate the function of natural teeth, with a strong, stable foundation that allows comfortable biting and chewing. In addition, nothing in the mouth looks or feels artificial.
- Increased stability and a sense of security that teeth will not fall out when eating, laughing or sneezing. People who wear dentures often worry that their dentures will fall out when they laugh, sneeze and sometimes even when they eat. Since the bone bonds to the implants, replacement teeth have a stable foundation and are securely attached to the implants, so there is no fear that teeth will fall out.
- Improved health due to improved nutrition and proper digestion. People with dentures usually have problems eating certain foods, such as fresh vegetables and fruits, which can compromise their nutrition. Additionally, since it is difficult to chew properly with dentures, digestion is often compromised.
- Improved appearance. Since implants preserve bone, preventing deterioration of the facial structures, appearance is improved. Collapse of the lower one-third of the face caused by complete tooth loss can be visually corrected and the remaining bone preserved. The appearance of wrinkles around the mouth caused by posterior bite collapse or complete facial structure collapse, are virtually eliminated. The smile is improved when replacement teeth look more like natural teeth. Even when only one tooth is missing, long term esthetics are usually much better with an implant-supported replacement tooth than with a traditional tooth-supported bridge. This is particularly important in the front of the mouth, where preventing a visible bone defect is critical for natural appearance.
- Improved ability to taste foods. Wearing an upper denture can prevent someone from really tasting food, as the roof of the mouth is covered. With implant-supported replacement teeth, it is not necessary to cover the roof of the mouth, so it is possible to enjoy the taste of foods.
- Increased convenience of hygiene. It is much easier to care for an implant-supported crown, which can be cleaned like a natural tooth, as opposed to a tooth-supported bridge, which requires the use of a floss threader for proper cleaning. It is also easier to clean implant-supported replacement teeth than a removable partial.
- Elimination of denture adhesives. Since implant-supported teeth are securely attached to the implants, there is no need for messy denture adhesives, which are often needed to keep dentures from falling out.
- Restoring self-confidence. Many of the people who now enjoy the benefits of implant-supported replacement teeth say their self-esteem has been restored as a result of improved appearance, function, comfort and health.
Nearly everyone who is missing one or more teeth and in general good health is a candidate for dental implant treatment. There are a few medical conditions that can undermine the success of implant treatment, such as uncontrolled diabetes and smoking. However, there are very few conditions that would keep someone from having implant treatment altogether.
Quality and quantity of available bone for implant placement is more often a factor in qualifying for dental implants than medical conditions. However, even people who have lost a significant amount of bone can qualify for dental implant treatment with additional procedures to add bone or create new bone. Advances in this type of treatment have made it possible for patients who would not previously have been considered candidates to have successful implant treatment.
Consultation. The first step is an examination and consultation to determine whether or not you are a candidate for implant treatment. This usually involves x-rays and may include taking impressions of your teeth. During the consultation we will be evaluating the area(s) of your mouth where teeth are missing, including the amount of bone available to support the placement of implants. We will also be evaluating the type of replacement teeth that will best meet your needs. A review of your health history will indicate whether there are any medical conditions that could prevent you from being a candidate for implant treatment.
Implant Placement Procedure. The implants are placed in the bone using a standard surgical technique. Following the implant placement procedure, the implants may be left undisturbed for a period of 3-9 months so that the bone can bond with the implants, or the implants may be placed and immediately “loaded” with replacement teeth. We will select the procedure that is best for you. In any case, you will always have the option of some type of temporary replacement teeth, so that you never have to be without teeth during treatment.
Abutment Attachment Procedure. Following the appropriate healing period, a small connector, or extension, called an abutment, is attached to each implant. Sometimes this is a temporary part used to help shape the gingival (gum) tissue and sometimes this is the “final” abutment. The permanent replacement teeth will eventually be attached to the abutments.
Fabrication of Replacement Teeth. A series of appointments with your dentist will be needed to take impressions of your teeth and the implant abutments, to place temporary replacement teeth, to select the appropriate shade for your replacement teeth, and to try them for proper fit. In between these appointments, the laboratory technician will fabricate your replacement teeth and the underlying structures that will be attached to the implants.
Dental implants preserve bone because they function like tooth roots, firmly embedded in the bone. In order for the implants to become embedded in the bone, the bone must bond to the implants. This process takes anywhere from 3 to 9 months, depending upon the quality of the bone into which the implants are placed. In selected cases, dental implants can be immediately loaded after placement. Thus, the time to complete this treatment plan is minimal.
There are other treatment options that do not include dental implants that do not take as long to complete; however, none of these traditional methods of tooth replacement preserve bone. And, in fact, dentures and partials accelerate the bone resorption process.
The home care recommended varies depending upon the type of implant-supported replacement teeth. For example, a single implant-supported crown is cleaned like a natural tooth, with regular brushing and flossing. Implant-supported bridges that replace a few teeth are cleaned like tooth-supported bridges, brushing and flossing with a floss threader.
Home care is a little different for people who are missing all of their teeth. Special brushes and floss are often recommended. With overdentures, it is necessary to clean the implant attachments, as well as the overdenture. Permanently fixed implant supported replacement teeth are cleaned like all other bridges.
In all cases, it is recommended that patients see their regular dentist and hygienist at least twice each year unless they routinely see the periodontist, in which case they would continue to alternate visits. If a surgical specialist placed the implants, it is usually recommended that the patient see the specialist at least once each year as well. These visits, combined with proper home care, are essential to the long-term success of implant treatment.
Documented clinical research demonstrates that implant-supported replacement teeth have been successful for over 35 years. These were some of the first root-form implant cases ever completed and they have been closely monitored from the beginning. It is highly likely that these cases will be successful throughout the lifetime of those patients.
Dental implants are designed to be permanent; however, many factors contribute to the long-term success of implant treatment, such as home care and regular maintenance visits to the dentist or dental specialist. By comparison, research demonstrates that the typical tooth-supported bridge lasts from 7-10 years and that partials and dentures are functional for approximately 5 years. Insurance statistics indicate that bridges, partials and dentures last 5 years and they generally pay for replacements every 5 years.
An investment in dental implant treatment is an investment in overall health, appearance and well-being, as it involves preserving the integrity of facial structures, as well as replacing missing teeth.
The actual cost of implant treatment is based on a number of factors, such as the number of missing teeth being replaced, the type of implant-supported teeth (treatment option) recommended and whether additional procedures are necessary to achieve the proper esthetic and functional result.
There is often a misconception that there is a set cost for each implant. The fees are calculated based on the amount of time the dentist or dental specialist anticipates spending to complete treatment (implant placement, other surgical procedures, fabrication of replacement teeth) as well as the estimated cost of implants, other components and materials necessary to complete treatment and dental laboratory fees.
The only way to accurately estimate the cost for an individual patient is to have an examination and consultation with us.